Are ACE inhibitors nephrotoxic

Elijah King
Published May 06, 2026
ACE inhibitors are not nephrotoxic. Baseline serum creatinine levels of up to 3.0 mg per dL (27 μmol per L) are generally considered safe.
Are ACE inhibitors bad for kidneys?
ACE inhibitors and creatinine Treatment with ACE inhibitors is associated with an acute increase in serum creatinine; a sign of mild kidney damage. Increased creatinine levels are attributed to the decline in the blood pressure in the kidney, caused by the inhibition of the renin-angiotensin system.
Are ACE and arbs nephrotoxic?
This triple therapy can increase the risk of acute renal failure. This triple therapy can increase the risk of acute renal failure.
Why do ACE inhibitors cause renal failure?
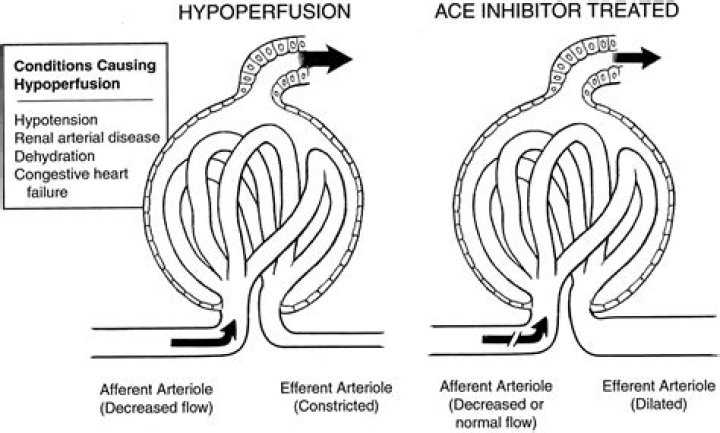
During ACEI initiation, renal dysfunction can occur due to a drop in renal perfusion pressure and subsequent decrease in glomerular filtration. This is attributed to the drug’s preferential vasodilation of the renal efferent arteriole, which impairs the kidney’s ability to compensate for low perfusion states.Are ACE inhibitors renal protective?
Because of their favorable intrarenal hemodynamic effects (particularly reduction of glomerular capillary pressure), ACE inhibitors may provide a renal protective effect in addition to their systemic antihypertensive effects.
When do you stop ACE in renal failure?
The decision to continue or discontinue ACEi/ARB use when patients reach CKD stage 4 or 5 is controversial. On one hand, risks associated with continuation include hyperkalemia, metabolic acidosis, and possible reduction in GFR.
What do ACE inhibitors do to GFR?
In general, ACE-inhibition does not affect normal glomerular filtration rate (GFR) but may increase GFR in patients on a low sodium intake prior to treatment. Since the rise in GFR is smaller than the rise in renal blood flow, in most instances a decrease in filtration fraction will result.
Do ACE inhibitors cause fluid retention?
In conclusion, angiotensin-converting enzyme inhibition can prevent the otherwise obligatory Na and water retention and systemic MABP increase during a 20% reduction in renal perfusion pressure. This is achieved most likely via the captopril-induced fall in angiotensin II and plasma aldosterone levels.Do ACE inhibitors cause vasodilation?
When used in congestive heart failure, ACE inhibitors exert a balanced vasodilator effect on arterial and venous beds and do not induce tachycardia or fluid retention. Cardiac output is increased whereas systemic vascular resistance, central pressures, and systemic blood pressure are reduced acutely and chronically.
What drugs are nephrotoxic?Drug class/drug(s)Pathophysiologic mechanism of renal injuryCisplatin (Platinol)Chronic interstitial nephritis, tubular cell toxicityInterferon-alfa (Intron A)GlomerulonephritisMethotrexateCrystal nephropathyMitomycin-C (Mutamycin)Thrombotic microangiopathy
Article first time published onAre ACE inhibitors contraindicated in pregnancy?
It is well accepted that angiotensin-converting enzyme (ACE) inhibitors are contraindicated during the second and third trimesters of pregnancy because of increased risk of fetal renal damage. First-trimester use, however, has not been linked to adverse fetal outcomes.
Who Cannot take ACE inhibitors?
- Pregnant women. …
- People with severe kidney failure. …
- People who have ever had a severe allergic reaction that caused their tongue and lips to swell, even if it was from a bee sting, should not take ACE inhibitors.
Why ACE inhibitors are not used in renal artery stenosis?
Angiotensin-converting enzyme inhibitors (ACEIs) are contraindicated in patients with bilateral renal artery stenosis due to risk of azotemia resulting from preferential efferent arteriolar vasodilation in the renal glomerulus due to inhibition of angiotensin II.
Is angiotensin II a vasodilator or vasoconstrictor?
Angiotensin II (ATII) is a very potent vasoconstrictor of the afferent and efferent arterioles, acting on two types of receptors, the AT1 and the AT2 receptor subtypes.
How are ACE inhibitors metabolized?
Most ACE inhibitors are eliminated mainly by the kidneys and to a lesser extent through the liver. Lisinopril is the only ACE inhibitor that does not require hepatic metabolism.
How do Diuretics cause vasodilation?
The direct vasodilator actions of thiazide diuretics on isolated vessels are associated with an increase in Rb+ efflux (as a marker for K+ efflux)1032 and hyperpolarization of the plasma membrane and are inhibited by selective blockers of the KCa channel.
Do ACE inhibitors cause ankle swelling?
Angiotensin-converting enzyme (ACE) inhibitors and angiotensin-receptor blockers (ARBs) are rarely associated with peripheral edema. If peripheral edema develops from the use of a calcium channel blocker (CCB), it is not on the basis of salt and water retention because this drug class is intrinsically natriuretic.
Why do vasodilators cause edema?
Vasodilatory edema, a common adverse effect of antihypertensive therapy with vasodilators, is related to several mechanisms, including arteriolar dilatation (causing an increase in intracapillary pressure), stimulation of the renin-angiotensin-aldosterone system, and fluid volume retention.
Are ACE inhibitors diuretics?
ACE inhibitor / thiazide diuretic combinations are used to lower blood pressure to treat hypertension. They work by relaxing blood vessels and by removing excess water and salt from the body.
Which medication is most likely to cause nephrotoxicity?
The most common drugs that cause DIKD include antibiotics, anti-rejection medications, antiviral agents, non-steroidal anti-inflammatory agents, anti-ulcer agents and chemotherapy. Most studies have defined nephrotoxicity as 0.5 mg/dL or 50% rise in Scr over 24–72 h time frame and a minimum 24–48 h of drug exposure.
What is the most nephrotoxic antibiotic?
The potentially nephrotoxic antibiotics in current clinical use are neomycin, kanamycin, paromomycin, bacitracin, the polymyxins (polymyxin B, and colistin), and amphotericin B.
Which drugs are contraindicated in renal failure?
Problematic drugs whose use in patients with renal insufficiency is nephrologically contraindicated: Pethidine, cefepime, lithium, gilbenclamide, gimepiride, metformin, spironolactone, eplerenone, methotrexate, gadolinium, enoxaparin.
Why is lisinopril contraindicated in pregnancy?
When lisinopril, or any ACE inhibitor, is taken during the second or third trimesters of pregnancy, it can cause low levels of amniotic fluid (the fluid that surrounds the baby). Low levels of amniotic fluid can lead to health problems for the developing baby.
Which drug is contra indicated in pregnancy?
DRUGS CONTRAINDICATED IN PREGNANCYThis chart represents information on select drugs that are contraindicated in women who are pregnant. Drugs that are contraindicated at a certain phase of pregnancy are noted.naproxen sodiumAleve, Naprelannaproxen/esomeprazoleVimovooxaprozinDaypro
Are ACE inhibitors teratogenic?
Specifically, these drugs were associated with increased infant risks for cardiovascular and nervous system anomalies. ACE inhibitors, long known to be teratogenic when used in the last two trimesters of pregnancy, have been considered safe in the first trimester.
Which is better ACE inhibitor or calcium channel blocker?
Studies in high-risk patients suggest that ACE inhibitors are superior to CCBs and other drugs in protection against cardiovascular events and renal disease.
How ACE inhibitors protect kidneys?
Treatment with ACE inhibitors results in kidney protection due to reduction of systemic blood pressure, intraglomerular pressure, an antiproliferative effect, reduction of proteinuria and a lipid-lowering effect in proteinuric patients (secondary due to reduction of protein excretion).
What is the difference between an ACE inhibitor and a beta blocker?
Beta-blockers treat many of the same conditions as ACE inhibitors, including high blood pressure, chronic heart failure, and stroke. Both types of medications also prevent migraines. Unlike ACE inhibitors, however, beta-blockers can help relieve angina (chest pain).
Why ACE inhibitors are contraindicated in aortic stenosis?
There is particular concern that vasodilators may lead to a reduction of the coronary perfusion pressure. In fact, the use of ACE-Inhibitors in aortic stenosis is classically considered to be contraindicated (3).
How do ACE inhibitors retain potassium?
ACE inhibitors and ARBs reduce proteinuria by lowering the intraglomerular pressure, reducing hyperfiltration. These drugs tend to raise the serum potassium level and reduce the glomerular filtration rate (GFR). Monitoring the serum potassium and creatinine levels and the GFR is therefore imperative.
What drugs are angiotensin receptor blockers?
- Azilsartan (Edarbi)
- Candesartan (Atacand)
- Eprosartan.
- Irbesartan (Avapro)
- Losartan (Cozaar)
- Olmesartan (Benicar)
- Telmisartan (Micardis)
- Valsartan (Diovan)